Home --> Diagnosis Wording --> Esophagus (To activate copy function, allow Adobe Flash to run)
Esophagus: Click sections headings below (in blue) to expand or collapse the content
 Diagnostic Headings (i.e. specimen & procedure)
Diagnostic Headings (i.e. specimen & procedure)
|
Diagnostic |
Headings |
|
|
|
|
Esophagus, at XX cm, biopsy: |
Esophagus, endoscopic mucosal resection: |
|
|
|
Distal esophagus, biopsy: |
Esophagus, gastro-esophageal junction, biopsy: |
|
|
|
Mid esophagus, biopsy: |
Esophagus, sub-site not specified, biopsy: |
|
|
|
Esophagus, segmental esophagectomy: |
Esophagus & proximal stomach, gastroesophagectomy: |
|
|
This subsection lists key diagnostic line for the most common diseases in this organ / system. Copy the relevant line(s) by clicking on the button and paste to your report to construct your own report. |
Normal and Inflammatory:
-- No diagnostic abnormality.
-- Moderate reflux esophagitis with intraepithelial esinophils (40 / HPF).
-- Moderate eosinophilic esophagitis with intraepithelial eosinophils (up to 40 /HPF).
-- Moderate erosive esophagitis associated with polarizable exogenous crystals, consistent with pill esophagitis.
-- Erosive esophagitis with fibrinoid purulent exudate, etiology uncertain.
Infectious:
-- Moderate acute fungal esophagitis, involving upper one-third of squamous epithelium.
-- Moderate herpesvirus esophagitis with mucosal erosion and fibrinoid exudates.
-- Severe cytomegalovirus esophagitis with mucosal erosion and granulation tissue.
Barrette's, Dysplasia and Carcinoma:
-- Gastric cardia-type mucosa with intestinal metaplasia and goblet cells.
-- Focal epithelial atypia indeterminate for low-grade glandular epithelial dysplasia.
-- Focal low-grade glandular epithelial dysplasia at squamous-glandular junction.
-- High-grade glandular epithelial dysplasia, at least 2.5 mm contiguous horizontal span, present in four of six microscopic fragments.
-- Invasive adenocarcinoma and extensive high-grade glandular dysplasia (see Note and Tumor Synopsis).
=============
Clinical scenario: 46-year old woman. Barrett's esophagus on endoscopy.
Distal esophagus, biopsy:
-- Benign esophageal mucosa with no histological abnormality.
-- No glandular component is present in this biopsy.
Slides examined: H&E x 1
CPT code: 88305 x 1
Editor's comment:
Reporting "No intestinal metaplasia" in a specimen composed entirely of squamous epithelium may be misleading. Specifying the absence of glandular component in the biopsy indicates inadequacy of the specimen and avoid a possible phone call to inquire where there is Barrett's.
=============
Clinical scenario: 16-yo girl, follow-up for eosinophilic esophagitis.
Distal esophagus, further designated as �GE junction�, biopsy:
-- Gastric cardia-type mucosa with minimal mononuclear infiltrate and reactive changes.
-- No mucosal erosion, intestinal metaplasia or increased stromal eosinophils.
-- No squamous/esophageal component is present in this biopsy.
Note: In the absence of squamous / esophageal component, possible eosinophilic esophagitis cannot be evaluated.
Slides examined: H&E x 1
CPT code: 88305 x 1
Editor's comment:
This example include typical structural components and format that are used widely -- Diagnosis Heading, Main diagnosis, applicable Note or Comment (e.g. stain results), Slides examined and CPT codes. For diagnosis with complex attributes (e.g. of resected malignant tumor), a synoptic report (or "Checklis") must be included to comply with ACoS mandates. To prepare "Synoptic Report" with an on-line tool, go to Home page and click on Tumor Reporting. It usually takes less than 30% of the time required by routine dictation method.
=============
Clinical scenario: 45-year old, nodular appearance on endoscopy. R/o cancer .
Distal esophagus, biopsy:
-- Nodular pancreatic metaplasia and mild chronic inflammation.
-- Focal foveolar cell hyperplasia
-- No active inflammation, intestinal metaplasia or glandular dysplasia.
Slides examined: H&E x 1
CPT code: 88305 x 1
Editor's comment:
None
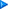 Non-specific Inflammation / Changes
Non-specific Inflammation / Changes
=============
Clinical scenario: 46-year old woman. R/o Barrett's.
Esophagus, lower third segment, biopsy:
-- Squamous-glandular junction with mild chronic inflammation.
-- No intestinal metaplasia, dysplasia or malignancy.
Editor's comment:
The histologic locale, " Squamous-glandular junction", indicates the sample adequacy for evaluation since absence of intestinal metaplasia in a specimen composed entirely of squamous epithelium may be misleading.
=============
Clinical scenario: 56-year old man. R/o eosinophilic esophagitis.
Distal esophagus, biopsy: #
-- Moderate lymphocytic esophagitis, etiology unknown (see Note).
-- Mild chronic gastric carditis with dense lymphoid infiltrates.
-- No eosinophilic esophagitis, intestinal metaplasia, dysplasia or carcinoma.
Note: Currently, lymphocytic colitis is largely considered a histological pattern rather than a specific etiological diagnosis. Underlying etiology largely remains uncertain. However, it has been reported that lymphocytic esophagitis can closely resemble eosinophilic esophagitis endoscopically and it is often difficult to distinguish these two by endoscopy. It is advised to report this diagnosis for correlation with the endoscopic finding.
Editor's comment:
Significant lymphocytic infiltrate in squamous epithelium, esp. when suspicious for eosinophilic esophagitis by endoscopy, should be reported although the cause is unknown.
=============
Clinical scenario: 53-year old man. R/o Barrett's.
Distal esophagus, "G-E junction", biopsy:
-- Mild chronic nonspecific gastric carditis.
-- No intestinal metaplasia, dysplasia or carcinoma.
-- No esophageal / squamous component is identified.
Editor's comment:
The histologic locale, " Squamous-glandular junction", indicates the sample adequacy for evaluation since absence of intestinal metaplasia in a specimen composed entirely of squamous epithelium may be misleading.
=============
Clinical scenario: 46-year old woman. R/o Barrett's.
Distal esophagus, at 40 cm, biopsy:
-- Squamous-glandular junction with mild chronic inflammation.
-- Mild reflux esophagitis with intraepithelial eosinophils (6/HPF).
-- No intestinal metaplasia, dysplasia or malignancy.
Slides examined: H&E x 1
CPT code: 88305 x 1
Editor's comment:
The histologic locale, " Squamous-glandular junction", indicates the sample adequacy for evaluation of Barrette's.
=============
Clinical scenario: 43-year old woman with dysphagia; r/o scleroderma.
Esophagus, GE junction, biopsies:
-- Moderate reflux esophagitis with intraepithelial esinophils (11 / HPF).
-- Mild chronic gastric carditis, nonspecific
-- No intestinal metaplasia, dysplasia or carcinoma.
-- No subepithelial stroma is present for evaluation of mucosal or submucal fibrosis
Slides examined: H&E x 1
CPT code: 88305 x 1
Editor's comment:
When clinical request is "r/o scleroderm", adequacy of the specimen (stromal presence) needs to be indicated. This is an example of report to answer clinical inquiry (see section of "Main Guidelines").
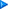 Intestinal Metaplasia and Barrette's Esophagus
Intestinal Metaplasia and Barrette's Esophagus
=============
Clinical scenario: 54-year old woman, h/o reflux and Barrett's, follow up.
Esophagus, biopsy:
-- Squamous-glandular junction with intestinal metaplasia, favor Barrett's esophagus.
-- No intraepithelial eosinophils, active inflammation, glandular dysplasia or carcinoma.
Slides examined: H&E x 3
CPT code: 88305 x 1
=============
Clinical scenario: 56-year old man with epigastric pain.
Esophagus, lower third, biopsy:
-- Squamous-glandular junction mucosa with mild acute and chronic inflammation, non-specific.
-- Separate fragment of gastric cardia-type mucosa with intestinal metaplasia and goblet cells (see Note).
-- No intraepithelial eosinophils, dysplasia or carcinoma.
Note: The intestinal metaplasia with goblet cells is present in cardia-type mucosa without connection to squamous epithelial component. If the specimen is from tubular esophagus, this finding may represent Barrett's esophagus. Alternatively, it may represent chronic gastritis with intestinal metaplasia if the biopsy is from gastric cardia. Correlation with endoscopic finding is necessary for this distinction.
Slides examined: H&E x 3
CPT code: 88305 x 1
Editor's comment:
Barrett's esophagus by definition is a disease of tubule esophagus and thus is NOT a diagnosis solely based on histologic findings.
=============
Clinical scenario: 46-year old woman. Barrett's esophagus on endoscopy.
Distal esophagus, at 38 cm, biopsy:
-- Squamous-glandular junction with prominent intestinal metaplasia and mild chronic inflammation, consistent with endoscopic finding of Barrett's esophagus.
-- Mild reflux esophagitis with intraepithelial eosinophiles (5 / HPF).
-- No glandular dysplasia or carcinoma.
Slides examined: H&E x 1
CPT code: 88305 x 1
Editor's comment:
Barrett's esophagus by definition is a disease of tubule esophagus and thus is NOT a diagnosis solely based on histologic findings. Given the endoscopic finding of "Barret's esophagus", this diagnosis can be rendered,
=============
Clinical scenario: 56-year old man with epigastric pain.
Esophagus, lower third, biopsy:
-- Gastric cardia-type mucosa with intestinal metaplasia and goblet cells (see Note).
-- No active inflammation, glandular dysplasia or carcinoma.
-- No squamous/esophageal component is present in this biopsy.
Note: The biopsy is entirely composed of glandular epithelium-lined mucosa. There is no squamous component in this specimen. If the biopsy is obtained from tubular esophagus, these findings may represent Barrett's esophagus. Alternatively, if the specimen is obtained from stomach, the finding is best categorized as chronic gastric gastritis with intestinal metaplasia. Correlation with endoscopic finding is required for such distinction.
Slides examined: H&E x 1
CPT code: 88305 x 1
Editor's comment:
Barrett's esophagus by definition is a disease of tubule esophagus and thus is NOT a diagnosis solely based on histologic findings.
=============
Clinical scenario: .
Esophagus, 32 cm, biopsy:
-- Gastric cardia-type mucosa with partial intestinal metaplasia, consistent with Barrett's esophagus.
-- No diagnostic abnormality in separate fragment of squamous epithelium.
-- No intraepithelial eosinophiles, dysplasia or malignancy.
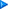 Eosinophilia and Eosinophilic Esophagitis
Eosinophilia and Eosinophilic Esophagitis
=============
Clinical scenario: 21-year old girl with dysphagia; follow up for eosinophilic esophagitis .
Esophagus, upper third, biopsy:
-- Moderate eosinophilic esophagitis with intraepithelial eosinophils (up to 40 /HPF) (see Note).
-- No stromal eosinophils or stromal fibrosis.
-- No mucosal erosion, significant neutrophilic infiltrates or fungal organism on GMS stain.
Note: The patient's recent prior esophageal biopsy (SP-15-031212, dated: 03/12/2015) with "eosinophilic esophagitis" is reviewed concurrently. There is apparent decrease, albeit mild, in the severity of the inflammation in the current biopsy, eosinophil count (40/HPF v.s. 69/HPF).
Slides examined: H&E x 1
CPT code: 88305 x 1; 88312 x 1
Editor's comment:
For a specimen of mid esophagus from a young patient with an established diagnosis, more important is to exclude infection and related sequelae such as erosion or stricture (fibrosis) than dogmatically state "no intestinal metaplasia, dysplasia.or carcinoma". Comparison with prior biopsy should be done to help assess efficacy of treatment.
=============
Clinical scenario: 18-year old girl with dysphagia .
Esophagus, upper third, biopsy:
-- Active esophagitis with intraepithelial eosinophils (up to 32 /HPF), highly suggestive of eosinophilic esophagitis. (see Note).
-- No mucosal erosion, polarizable crystals deposits, significant neutrophilic infiltrates or stromal fibrosis.
-- No fungal organism is identified on GMS stain.
Slides examined: H&E x 1
CPT code: 88305 x 1; 88312 x 1
Editor's comment:
Relevant negative findings (line-2) indicating the absence of other common causes (i.e., chemical, infection) in the differential diagnosis should be included in report. For a specimen of mid esophagus from a young patient, more important is to exclude infection or related sequelae such as erosion or stricture (fibrosis) than dogmatically state "no intestinal metaplasia, dysplasia.or carcinoma".
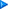 Dysplasia (Glandular or Squamous)
Dysplasia (Glandular or Squamous)
=============
Clinical scenario: 47-year old man with reflux disease and Barrette's. r/o dysplasia.
Esophagus, at 33-36 cm, biopsy:
-- Focal epithelial atypia indeterminate for low-grade glandular epithelial dysplasia (see Note).
-- Extensive intestinal metaplasia with goblet cells.
-- Moderate acute inflammation associated with epithelial atypia.
-- No high-grade epithelial dysplasia or carcinoma.
Note: Sections reveal extensive intestinal metaplasia with focal glandular epithelial atypia associated with acute inflammation. It is difficult in this case to segregate reactive atypia from low-grade epithelial dysplasia due to significant acute inflammation.
Slides examined: H&E x 1
CPT code: 88305 x 1
Editor's comment:
When findings are indeterminate for dysplasia, report should indicate the reason(s) (e.g. inflammation, sample size ect.) why a definitive diagnosis cannot be made.
=============
Clinical scenario: 57-year old man; follow-up for Barrette's.
Esophagus at 30-33 cm, biopsy:
-- Focal low-grade glandular epithelial dysplasia at squamous-glandular junction.
-- Extensive intestinal metaplasia with goblet cells.
-- No mucosal erosion, acute inflammation, high-grad dysplasia or invasive carcinoma.
Slides examined: H&E x 1
CPT code: 88305 x 1
Editor's comment:
Diagnosis of low-grade glandular epithelial dysplasia is associated with high degree of inter- and intra-observer variability and is often affected by co-existent histological processes such as acute inflammation. Indicating whether these interfering factors are present (line-3) can help reader assess the accuracy of the key diagnosis.
=============
Clinical scenario: 72-year old man. h/o Barrette's and dysplasia.
Distal esophagus, biopsy:
-- High-grade glandular epithelial dysplasia, at least 2.5 mm contiguous horizontal span, present in four of six microscopic fragments.
-- Cannot entirely exclude focal early intramucosal adenocarcinoma.
Slides examined: H&E x 2
CPT code: 88305 x 1
Editor's comment:
Although "early intramucosal adenocarcinoma cannot be entirely excluded" (for line-2) may be more grammatically correct, statement with leading negation is preferred (see section of "Science behind").
 Erosive Esophagitis (Including Pill Esophagitis)
Erosive Esophagitis (Including Pill Esophagitis)
=============
Clinical scenario: 63-year old woman with dysphagia.
Esophagus, biopsies:
-- Erosive esophagitis with fibrinoid purulent exudate, etiology uncertain (see note).
-- No polarizable exogenous material, viral cytopathic changes, dysplasia or carcinoma.
-- No fungal organisms are identified on GMS stain.
Note: The main differential diagnosis for the erosive esophagitis should include pill-induced injury, infection, ischemia and malignancy. Although a pill-induced erosive esophagitis is strongly favored, other possible etiologies cannot be entirely excluded.
Slides examined: H&E x 1; 1 GMS x 1.
CPT code: 88305, 88312
Editor's comment:
None.
=============
Clinical scenario: 81-year old woman with dysphagia. R/o cancer .
Esophagus, mid third, biopsy: Clinical scenario: 81-year old woman with dysphagia. R/o cancer .
-- Moderate erosive esophagitis associated with polarizable exogenous crystals, consistent with pill-induced esophagitis (see Note).
-- No viral cytopathic changes, dysplasia or carcinoma.
-- No fungal organisms are identified on special stain.
Note: The constellation of mucosal erosion, presence of exogenous crystal admixed in the exudate, and a few intraepithelial eosinophils in adjacent squamous lining is consistent with pill-induced esophagitis. Correlation with endoscopic findings and clinical history to confirm the histologic diagnosis is recommended.
Slides examined: H&E x 1; 1 GMS x 1.
CPT code: 88305, 88312
Editor's comment:
Fibers of specimen carriers (e.g., paper) is also polariable but they are NOT crystaloid. Although pill-induced esophagitis is most commonly seen in elderly, other common causes of erosive esogaphagitis (such as infection and carcinoma) must be considered and excluded.
=============
Clinical scenario: 79-year old man with dysphagia .
Mid esophagus, biopsy:
-- Moderate acute fungal esophagitis, involving upper one-third of squamous epithelium.
-- Innumerable yeast and invasive hyphae forms of fungi are revealed by PAS-D stain.
-- No mucosal erosion, viral cytopathic changes or polarizable exogenous material.
-- No dysplasia or carcinoma.
Slides examined: H&E x X
CPT code: 88305 x 1
Editor's comment:
Fungal invasion of epithelial layer and associated acute inflammation are required for fungal esophagitis and distinguish it from contamination by oral flora. Such contamination is also often seen in mucosal ulceration associated with other causes such as pill esophagitis and carcinoma. Thus, line-3 is included in report to indicate whether such a cause is present.
 Viral Esophagitis (HSV and CMV)
Viral Esophagitis (HSV and CMV)
=============
Clinical scenario: 32-year old woman with dysphagia. Geographic ulcer, ? fungal infection.
Esophagus, lower third, biopsy:
-- Moderate herpesvirus esophagitis with mucosal erosion and fibrinoid exudates.
-- No fungal or eosinophilic esophagitis.
-- No fungal organism is seen on GMS stain.
-- No gastric/glandular component is present.
Slides examined: H&E x X
CPT code: 88305 x 1
Editor's comment:
This section critics on the pro & con of the the wording. There will be 12-pt space after text paragraph.
=============
Clinical scenario: 22-year old man. h/o leukemia; s/p bone marrow transplant. r/o GVHD
Esophagus, lower third, biopsy:
-- Severe cytomegalovirus esophagitis with mucosal erosion and granulation tissue, diagnosis confirmed by immunohistochemistry.
-- No graft-versus-host disease (GVHD).
-- No fungal organism on GMS stain.
-- No herpesvirus cytopathic changes.
Slides examined: H&E x 1
CPT code: 88305 x 1, 88342 x 2, 88312 x 1.
Editor's comment:
In immune-compromised patient, commonly encountered infections at this site should be investigated and the results be included in the report.
=============
Clinical scenario: 72-year old man; h/o prostatic cancer. friable mucosa, r/o infection or malignancy.
Distal esophagus, biopsy:
-- Severe acute esophagitis with mucosal erosion and purulent exudate.
-- Granulation tissue with cytopathic changes suspicious for but not diagnostic of cytomegalovirus infection (CMV esophagitis) (see Note).
-- No herpesvirus (HSV) is identified by immunohistochemical stain.
-- No fungal organism is seen on GMS stain.
-- No polarizable exogenous crystal material, epithelial dysplasia or carcinoma.
Note: The specimen is largely composed of purulent exudate and necrotic tissue. A small fragment of granulation is noted to have focal cytopathic changes suggestive of viral inclusion. Such changes disappear on a different plane of section and result of immunohistochemical stain for CMV is equivocal. Thus, a definitive diagnosis of CMV esophagitis cannot be rendered. Serological work-up is recommended to aid the diagnosis.
Slides examined: H&E x 2
CPT code: 88305 x 1, 88312 x 1, 88342 x 2
Editor's comment:
An elderly patient with history of malignance should be suspected to be immune-compromised. Commonly encountered infections in such a patient (i.e., CMV, HSV and fungus) should be investigated and the results should be reported. Pill esophagitis frequently associated with mucosal erosion should also be considered.
=============
Clinical scenario: 73-year old man with long standing Barret's. Recent high-grade dysplasia on biopsy.
Distal esophagus, endoscopic mucosal resection:
-- Invasive adenocarcinoma and extensive high-grade glandular dysplasia (see Note and Tumor Synopsis)
Slides examined: H&E x 3
CPT code: 88307 x 1
Editor's comment:
Report of invasive carcinoma in specimen obtained by endoscopic mucosal resection (EMR) should include the following tumor attributes: (i) depth of infiltration, differentiated as m1�m4 and sm1�sm3; (ii) evaluation of the resection margins, lateral and deep (R0/R1); (iii) degree of differentiation (G1�G4) and (iv) invasion of lymphatic or blood vessels. (Good handling and pathological examination of endoscopic resections of early Barrett's cancer. Diagnostic Histopathology. (18)12: 2012).
=============
Clinical scenario: 46-year old woman. R/o Barrett's.
Distal esophagus, biopsy:
-- Invasive adenocarcinoma, moderately differentiated, at least 6 mm, fragments of
--
Note: Immunohistochemical studies show that the tumor cells are positive stain of the tumor cells for PMS-2, MSH-2, MSH-6, and MLH-1. This staining profile indicates that there is no loss of expression of major mismatch repair proteins.
Editor's comment:
None
Hidden Paragraph text goes here
=============
Clinical scenario: 41-year old man. Nodule in upper essophagus.
Esophagus, upper third, endoscopic mucosal resection:
-- Granular cell tumor, 6 mm on the plane of section, focally involving one end margin.
-- Deep margin is free of the tumor.
-- Diagnosis confirmed by positive immunohistochemical stains for S100 and CD68.
-- No mucosal erosion, epithelial dysplasia or carcinoma.
Slides examined: H&E x 3
CPT code: 88307 x 1
Editor's comment:
Report of invasive c
Hidden Paragraph text goes here
Hidden Paragraph text goes here